|
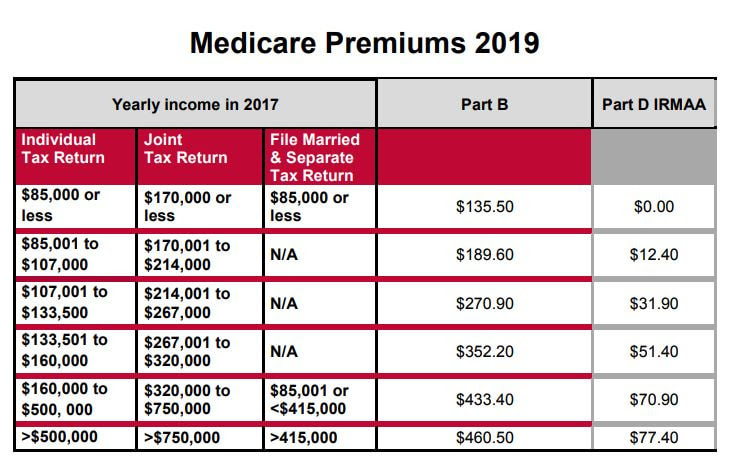
Last week, the CMS (Centers for Medicare & Medicaid Services) released the 2019 premiums for Medicare Part B & D. The chart below demonstrates the 2019 Part B Premiums to be paid by individuals depending on their household income as well as the 2019 Part D income-related monthly adjustment amounts. In addition, please note that for Part D Medicare prescription programs, after total retail costs for your prescriptions reach $3,820 (for 2019), you will pay no more than 37%coinsurance for generic drugs or 25% coinsurance for brand name drugs until you have paid a total of $5,010 (for 2019). Medicare Annual Enrollment Period runs from now until December 7th. Don't navigate through the Medicare Maze alone. Our Experts are your resource to answer any questions you may have during the busy season.
1 Comment
The Federal Mandate works to level the playing field while providing care to everyone, including those with pre existing conditions, to avoid insurers "cherry-picking" healthy members. To accomplish this, a portion of the revenue from the companies with healthier members goes to the companies with less healthy members. However, defects in the small-group program have resulted in New York’s smaller, more-innovative insurers like CareConnect to subsidize larger competitors.
The Direct Effect to Northwell CareConnect CareConnect has to make a significant transfer of revenues as mandated by the Affordable Care Act. To illustrate: Care Connect has approximately 7% in fixed costs, 80% in medical expenses, along with state and federal taxes of 5%. This illustrates that CareConnect is doing well and would generally lead to a slight increase if any. However, In 2016 with revenues of approximately $700,000,000, CareConnect’s Federal Risk Adjustment liability is $112,000,000 92% of that revenue transfer is going to Oxford which maintains approximately 55% of the total NYS market. In the downstate area (which most of us live in) they represent 70% of the market. Right now, Northwell CareConnect has the most cost effective plans in each of the Metallic Levels. CareConnect with other organizations are trying to have this mandate repealed for the small group marketplace (2‐100 ee’s on the payroll). It is creating a burden on small businesses and their employees along Main Street. If the Federal Risk Adjustment mandate were to be repealed, executives at CareConnect stated they would apply for a minimal increase, if any. So far the Mandate remains, causing Northwell CareConnect to request withdrawal from the health insurance marketplace. CareConnect operations will continue over the next year as the company works with its customers, businesses and others to help transfer policy holders to other health plans. Throughout the transition, CareConnect will continue to pay claims and serve members, patients and providers. Optimistically, we are hoping for a change of heart from the ACA. This directly affects hard working New Yorkers trying to obtain quality affordable coverage.
So much of life, work, family and entertainment now takes place online, so it’s no surprise healthcare delivery is increasingly happening online as well.
There were 1 million virtual doctor visits in 2015 Why?
Who can benefit?
Most of us at some point in time have had to select a health insurance plan. There are many factors to consider in order to select the plan that is right for you. At Mainline insurance we conduct a full needs assessment before we even begin to look at plans. That way we show you plans that make sense and remove the plans that are not really an appropriate option.
A simple needs assessment is conducted in a few minutes. We evaluate your health, income, age, eligibility and provider network preferences. First is your overall health, how often do you see a doctor? once a year? once a month? Do you see any specialists or take any medications on a regular basis. If so are these medications generic or specialty drugs? Let's say for example you are healthy, a physical once a year and the occasional cold. It may make sense for you to lean towards a lower premium plan at the catastrophic, bronze or silver level. All ACA plans include free preventative care (physical, blood work, usually a free doctor visit) For a healthy individual this may be suitable for your needs and save you money with lower monthly premiums while still providing max out of pocket protection in the event of something catastrophic happening. Alternatively, maybe you see a doctor often, perhaps you are diabetic. Typically, people in this situation require multiple specialist visits a year, monthly medication and durable medical equipment. For these individuals it makes sense to do a platinum level plan. Although premiums are much higher, the max out of pocket is lower and in the long run you will actually save money as you engage the healthcare system. In the individual market, income is important. For an individual in New York earning between $16k and $46k/year you will likely qualify for subsidies in the form of Advanced Premium Tax Credits. These APTCs will reduce your monthly premiums by an amount dependent on you income. It is important to consult a professional so they can assess your income accurately and get you the appropriate tax credit amount. Age does make a difference, If you are younger than 30 you have plan options that are relatively inexpensive, so if you are healthy they may be the most economical option and provide only the coverage you need instead of paying for services you won't use. For older individuals you may think, "Well I'm healthy, I don't need a high level plan." This may be true, but keep in mind as you get older, things break, that's life unfortunately. In that case it may be worth it to have the security of a gold or platinum plan. Eligibility is a big factor. During Open Enrollment, which is between November and February anyone can freely purchase or change health insurance plans without restriction. However, if you are outside of this time period in what's call Special Enrollment, you will need to have what is called a Qualifying Life Event. This is typically an involuntary loss of coverage (ex. lost a job, lost coverage). There are other's but we will save them for another day. Finally, we look at provider network. If you are seeing a doctor or prefer certain doctors and hospitals its important we consider only plans that cover those physicians. At Mainline we have the resources to determine which doctors are in a plans network and which ones are not. Let us do the research for you. If this all seems too complicated and too labor intensive don't worry, we have licensed brokers standing by ready to assess your needs and find the plan that's right for you. Voluntary benefits are insurance products that employers offer to employees, with the cost assumed by employees who elect the coverage. Typically, these packages include coverages such as dental, vision and disability. When employees obtain these products through their employer, the rates are lower than employees could get if they purchased them on their own. Many times they are not available on a non-group basis. Employers offer voluntary benefits because they allow companies to provide a better benefits package at no additional cost to them. The types of Voluntary Benefits are:
Dental, Vision, Short Term Disability, Long Term Disability, Life Insurance Dental insurance is designed to pay a portion of the costs associated with dental care. Generally dental offices have a fee schedule, or a list of prices for the dental services or procedures they offer. Dental insurance companies have similar fee schedules which is generally based on Usual and Customary dental services, an average of fees in your area. The fee schedule is commonly used as the transactional instrument between the insurance company, dental office and/or dentist, and the consumer. Vision insurance and vision plans can lower your cost of eye care and prescription eyewear. Vision insurance is an optional health policy that entitles you to specific eye care and eyewear benefits defined in the policy. Short Term Disability Insurance can replace a portion of your income during the initial weeks of a disabling illness or accident. Policies can cover from the first 6 months up to a year of a disability, providing coverage during the waiting period of most Long Term Disability Insurance plans. Once the short-term benefits expire (generally after three to six months), long-term disability insurance pays a percentage of your salary, usually 50 to 60 percent, depending on the policy. The benefits last until you can go back to work or for the number of years stated in the policy. Life Insurance is a contract between an insurance policy holder and an insurer or assurer, where the insurer promises to pay a designated beneficiary a sum of money (the benefit) in exchange for a premium, upon the death of an insured person (often the policy holder). Depending on the contract, other events such as terminal illness or critical illness can also trigger payment. The policy holder typically pays a premium, either regularly or as one lump sum. Other expenses (such as funeral expenses) can also be included in the benefits. How will the government know who has coverage through their job? Simple, sort of. Employers are required to complete the 1094C ACA Compliance draft form. It is called the transmittal of employer provided health insurance offer and coverage information returns. It will be used to identify employees on payroll that are receiving health coverage. It is also accompanied by a 1095C form to be filed by ALE members which is the Applicable Large group Employer(50+ employees on payroll). The Internal Revenue Service has issued draft versions of the reporting forms. Most employers will begin using the forms next year to show that their group health insurance plans comply with the health care reform law. The long-awaited draft forms are the first practical application of employers' health care coverage and enrollment reporting obligations under the Patient Protection and Affordable Care Act since the regulations were finalized in March. The forms are the primary mechanism through which the government intends to enforce the health care reform law's minimum essential coverage and shared responsibility requirements for employers. Beginning in 2015, employers with at least 100 full-time employees will be required to certify that benefits-eligible employees and their dependents have been offered minimum essential coverage. Their employees' contributions to their premiums must comply with cost-sharing limits established under the reform law. Smaller employers with 50-99 full-time employees are required to begin reporting in 2016. Additionally, self-insured employers will be required to submit documentation to ensure compliance with minimum essential coverage requirements under the reform law's individual coverage mandate. Download the 1094C ACA Compliance Form Draft below. This form is a draft and not to be used for filing. The purpose is to give employers a better understanding of the program requirements and prepare them for compliance in 2015. As always Mainline Insurance is on your side and ready to assist in form preparation and enrollment.
 Beginning January 1, 2014, all current Emblem plans (including the GHI Healthy NY EPO and HIP Healthy NY HMO) will end. At this time, new plans will be offered. For Clients that have Emblem through HealthPass or the LIA, existing plans will be mapped to a different plan being offered. All new Emblem plans will meet the 10 essentials benefits that are now required by the Affordable Care Act. The benefits and rates for all the new Emblem HMO plans (including Healthy NY) are attached to this distribution. The Affordable Care Act, requires benefits such as physical therapy, mental health/substance abuse treatment, chiropractic, and durable medical equipment to be included in the Healthy NY Plan. The network of doctors and hospitals on these plans have also changed. If continuing your current physician relationship is important to you, we suggest contacting your physician’s office to see if they participate in the new network. The name of the new network is Select Care. If your physician already participates in the Select Care Network or you are willing to change physicians, this plan is a viable cost effective option. It should be noted that this plan has a significantly smaller physician network. If you wish to choose any of the new Emblem plans for January 1, 2014, you are required to fill out new applications to reapply. The Emblem Healthy NY Plan, while competitively priced, has a smaller network than previous. We are here to help you, with this transition of benefits. Mainline Insurance will review all of the options available to you and synthesize the optimal individual solution. We are very sensitive to our client’s benefit needs and budgets. If obtaining benefits on the New York State Health Benefit Exchange is the most viable option, Mainline Insurance is certified and authorized to help you with this at no additional cost. For clients that have Emblem and are billed directly from Emblem, additional steps must be completed or no coverage will be effective for January 1, 2014. It has been difficult due to technical malfunctions and insurance network changes to identify participating physicians. We hope to see these issues remediated over the next few months. However, for the present time please check directly with those providers that are vital to your well being about which networks they participate in. This is very important as we previously mentioned, networks have changed significantly. Click To Download 2014 Emblem HMO Plan Design And Rates Click To Download 2014 Emblem Healthy NY Rates Click To Download 2014 Emblem Healthy NY Plan Design is a key component of the Affordable Care Act.
Purpose: To help covered individuals and families with the out of pocket expense when they access care. How Does Someone Qualify?
Example: This example is an approximation.
If you fall into the 200-300 of FPL category you would qualify for a 50% reduction. This would mean the maximum you would pay out of your pocket for co-pays and deductibles would be $3,125 for a single or $6,250 for a family. The Cost Sharing Subsidy is a key component in the new Affordable Care Act to help making healthcare affordable. Regards, Vincent  This months marks the start of open enrollment. You will have the opportunity to change plans if you are unhappy with the one you are currently on. Medicare Open Enrollment Period: October 15th, 2013 through December 7th 2013 If you have a Medicare Supplement Plan here are some of your options.
The Medicare Advantage PPO and HMO Programs have networks to access to receive the most cost effective care. The Medicare Advantage program allows you to go outside the network but with higher out of pocket costs If you have a Medicare Advantage PPO here are some of your options.
Best Regards, Vincent Reda |
AuthorMainline President Vincent Reda is a Healthcare specialist with 40 years of experience in providing healthcare coverage to individuals and organizations. Categories
All
Archives
October 2018
|
||||||
Call us today(631) 543-5242Speak with a Licensed Insurance Agent
Mon-Fri 9am-6pm |
|
Mainline Insurance Inc.
366 Veterans Memorial Highway, Suite #4 Commack, NY 11725 Home | Privacy Policy | About Us | Credits Copyright © 2022 |




 RSS Feed
RSS Feed